So you’ve got a chronic illness? Shit’s about to get real. Here’s something I can say with completely certainty: the “system” (multiple systems) can, and will, let you down. You need to learn how to advocate for yourself, and how to accept help from others to do the same. Being sick, and being a self-advocate, is a full-time job. The only pay-off is keeping your head above water.
I generally try not to write things that are completely negative. However, as you can probably tell, I’m in a very negative headspace right now. I think the stories I am about to tell will go some way to showing you why.
Chronic illness, in and of itself, is exhausting. Even when whatever diagnosis you have isn’t completely debilitating, even when you’re making headway, even when you have a lot of help. It. Is. Exhausting.
And when you add on top of that the fact that it is almost entirely up to you to manage:
- Medication
- Side effects from medication
- Scripts and visits to the pharmacy
- Diet
- Exercise
- Doctor’s visits
- Specialist visits
- Multiple treatments and therapies
- Your mental health
… you can see why it starts to feel like it’s All Too Much.
Before I got sick, four and a half years ago, I had zero idea of what living with chronic illness would be like. Why would I? I was pretty healthy, if a bit fragile occasionally. Most people who’ve never been chronically ill can not, and will never, really grasp what this life is. I don’t blame for that. I envy them.
One of the main conclusions of Stephanie de Montalk’s PhD into chronic pain was that this experience only makes sense to fellow

Steph de Montalk at work
sufferers. There is no real way of crossing that language barrier between the able and the disabled.
However, I’m going to try, a bit. I’m going to give a description of my life over the past four and a half years, in very simplistic terms. This account should go some way to explaining what I mean when I say being sick is a fulltime job. I spend hours every single week seeing doctors, having treatments, resting, recuperating, fighting, pushing through, making trips to the pharmacy, and making follow-up phone calls to various parts of the incredibly complex medical system – because if I don’t, nothing will happen. I’m serious.
As an able person, I assumed that doctors and medical staff were always on the ball. They had good, robust, fairly automated systems in place that were there to put patients first, even if the occasional human mishap occurred.
My own experience, and that of many, many other people that I have met over the past four years, has proved to me that that’s wrong. I was wrong.
“Mishaps” happen constantly. If you don’t know to expect that, and if you don’t learn how to advocate for yourself: you’re going to slip through the cracks. You’re going be left behind. You’re going to become a statistic.
ONE: Let’s do a quick walk-through of some of the things that have happened to me because of the medical system since July 2012.
1. I got sick, and it took three doctors and six months to figure out what was wrong with me.
2. They treated me with a series of harsh antibiotics, ruining the fragile balance of my gut flora. Despite textbook circumstances and symptoms, the doctor did not check for a clostridium dificile infection until a month later. By that time, I was hospitalised with toxic megacolon.
3. I was told I likely had Ulcerative Colitis, and I needed an urgent colonoscopy to confirm this.
4. When I left hospital, I wasn’t given half the medications I was supposed to have, so I spent several weeks untreated.
5. During those weeks, I researched UC and came to grips with it. I was yet to hear about my colonoscopy, so I rang the hospital to find out where I was on the list. They had no record of me. It turned out of the order for the procedure had been misfiled and I wasn’t on the list at all. If I hadn’t called, I’d never have gotten one.
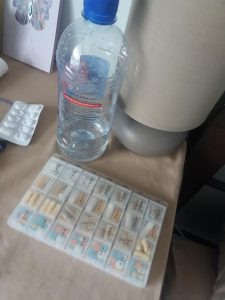
A regular week
6. After the colonoscopy, I was told I didn’t have UC after all, I “just” had IBS as a result of the antibiotics and subsequent infections. The gastroenterologist said it might take 6 months to a year for me to recover.
7. I did not recover. The pain spread and became excruciating in my spine. Finally, my GP tested for the HLA-B27 gene to see if it was possible I had Anklylosing Spondylitis. The test was positive. At this point I’d been sick for over two years.
8. I find out I can’t access treatment for AS without an MRI showing the damage in my spine. The waiting list is around six months. I raised money to get the test privately. (Same machine, same doctors. One of the reasons the public waiting list is so long is because time is booked out for people who can pay upward of $1300).
9. The first two drugs they try me on make little difference. (Humira, Enbrel). In November 2016, rheumatology finally agrees that the drugs are not working, and the side effects mean I need to look at infusions of a new medication given at the hospital. They ask me to wait a further three months “just to make sure.” My symptoms get worse.
10. My February appointment was never made. I only get one because I call several times to ask where I am on the list. At this appointment (Friday 27 February this year), the nurse agrees it’s time for infusions. She says she’ll call me on Monday to tell me exactly which medication that will be.
11. I wait til Wednesday and hear nothing, so I start calling. No one ever answers at the clinic so I leave message after message.
13. On Tuesday 14 March, I get a voice mail from the receptionist at the clinic. They say the nurse met with the doctor yesterday (two
weeks after I was told that would happen), and the doctor has prescribed something for me.
14. I’m not expecting a prescruption. I have no idea what the voice mail means, but it seems clear to me that no one at the other end really knows either, and had I not continuously called, I may never have heard anything. The nurse has never called to explain or discuss anything with me. Had I not made a nuisance of myself, I may never have heard anything at all.
15. Wednesday 15 March. The receptionist tells me that there’s no intention to move me to an infusion, despite me now
waiting four months for this to happen. The script I’ve been given is for a medication that’s been tentatively tested in a very small group of people to treat fibromyalgic pain. I never reported an increase in fibro symptoms (I also tend to think that my diagnosis of fibromyalgia is very secondary to my AS, and that that diagnosis in itself is a very weak one. “Fibromyalgia” is the name given a bunch of pain and fatigue symptoms that doctors cannot otherwise explain. I’m not saying it’s not real. It just does zero good to me as a label).
16. I cry when I hang up the phone. All this energy from me, for nothing. Why am I not being given the infusions? Why has no doctor ever called me? The script is not only likely to make some of my symptoms worse, it does nothing to address the debilitating side effects of the Enbrel I’m currently on. It may well have pain benefits: but am I willing to take that chance when no doctor has taken the time to explain it to me?
NB: I’ve asked a friend to step in as an advocate for me on this one, because I am totally burned out on it.
I also want to recognise that everyone I’m talking about here is an actual person, and people deserve empathy, even when they’re not doing what you need. The receptionist here isn’t being put in a good position; they shouldn’t have to be passing on medical info in this way. People are often doing the best they can within a very underfunded system.
So now we get to here. I’m going to leave the physical health sector for a second and skip on over to mental health, although I a) Think it is wrong to treat them as two separate things, and b) Don’t want to talk too much about my personal MH history.

An image of illness by artist Jem Yoshioka
TWO: Self-advocating in mental health
If you think it’s hard advocating for yourself in a physical health context, when you’re exhausted and in pain, consider it approximately a billion times harder with mental health.
I have a large network now of people I know suffering chronic physical illness. All of them also suffer chronic mental illness. It’s not surprising, is it, when you look at all of the above, and you consider how depressing it must be to live like this, and how anxiety-provoking it must be to constantly try and stand up for yourself.
So, you’ve got a physical illness. The likelihood of being told that it’s “all in your head,” is, statistically, Extremely Fucking High. (Especially if you’re a woman. Examples: X, X, X). Again, I know this because of my own experiences, and those in the large network I am part of. I know this because Stephanie de Montalk has written and talked about it. I know this because I lost a friend last year who was told one too many times that her pain wasn’t real.
If a doctor’s starting point is to believe that you’re making shit up… getting help is going to be kind of a problem.
There’s some reasons I have been able to access the level of mental health assistance I need.
- I’m articulate. I’m educated, and my education happens to be in communications. People take me seriously because I know what language to use to get them to do so.
- My education also means I can research what help is available and follow it up – ie counselling paid for by ACC, what rights I have through my GP and who they can refer me to, what free or private services I can seek.
- I’m white. Despite being overrepresented in mental health data in New Zealand, Maori and Pacific people do not get the same help. (Some good information on this is available from the Mental Health foundation here, and from the Ministry for Health here).
- I have just enough financial means – ie, I can access the internet, I can visit my GP, I can pay for prescriptions.
- I’m stubborn.
I am extremely privileged to be getting the level of help I am currently getting, because I need it. I recognise that so many people are not getting that help, maybe because they don’t have or can’t do one or all of the above. What happens to those people? They slip through the cracks. They get left behind. They die.
There’s a reason New Zealand has one of the highest suicide rates per capita in the developed world.
THREE: Another system in which I constantly have to self-advocate: WINZ.
I’ve talked a lot about this over the past four years, since I first had to apply for what was then a sickness benefit. So I probably don’t need to go into detail here.
The five reasons above also apply to this situation. I have been able to self-advocate because I’m educated, because I can research my  rights, because I’m white, because I have financial means, and because I am stubborn. I can also add to that that I was able to get my story into the media and therefore force WINZ to act or face public consequences. That was dumb luck, really.
rights, because I’m white, because I have financial means, and because I am stubborn. I can also add to that that I was able to get my story into the media and therefore force WINZ to act or face public consequences. That was dumb luck, really.
If that hadn’t happened, I’d probably still be scrabbling hard to get everything I am entitled to. I know that this is the reality for thousands of people.
I want to be well enough to be an advocate for others. To put everything I’ve learned to use not just for myself, but for so many people who suffer. It’s not possible right now, but it may be in the future. I’m not trying to be self-righteous. I’m not saying I’d do it tirelessly and for free. But that’s the reason I write things like this. Because it’s the only means I have of trying to spread information and encouragement. Of showing people they’re not alone, they’re not imagining things, and they are entitled to help.
Being chronically ill is hard enough all on its own. When you suddenly realise how much of your incredibly precious energy, hours, and resources – things you probably took for granted when you were well, if you ever were – when you realise how much of all that is used up just fighting to get anything from the systems that you thought were built to support you?
It’s deeply, deeply traumatising.
Again. I feel so incredibly lucky that I have the ability to communicate, to be stubborn, and have access to the support network I have. I worry constantly about the people who don’t have those things. How do they survive? How many of them just slip through the cracks?
We know the answer. Too many.
If you feel like supporting me and this writing
You can do so by buying a copy of Skeletal Mosaic, or becoming a patron on Patreon. Thank you.

Design by Jem Yoshioka
